Every evening a remarkable process repeats itself: your body begins to cool from the inside. Core body temperature drops from around 37.0 °C in the afternoon to a minimum of about 36.2 °C in the early morning hours. This temperature drop is not the consequence of falling asleep – it is a prerequisite for it.
The two-process model
Sleep researcher Alexander Borbély described a model in 1982 that remains the foundation of sleep research to this day: the two-process model. It explains why you become sleepy in the evening and wake in the morning – through the interplay of two independent mechanisms.
Process S – Sleep pressure
Process S (S for "sleep" or "somnogenic") describes homeostatic sleep pressure. It builds with every hour you are awake. The longer you stay awake, the stronger the urge to sleep. The main driver is the accumulation of adenosine in the brain – a metabolic by-product that builds up during wakefulness and is broken down during sleep. Caffeine blocks adenosine receptors, which is why coffee keeps you awake.
Process C – The internal clock
Process C (C for "circadian") is the internal clock with a rhythm of roughly 24 hours. It is controlled by the suprachiasmatic nucleus (SCN) in the hypothalamus and synchronised by light entering the eyes. Process C determines when the body is programmed for activity and when for rest – regardless of how tired you are.
Sleep is initiated when two conditions are met simultaneously: high sleep pressure (Process S) coincides with low circadian wake promotion (Process C). For most people this moment falls between 10 pm and midnight.
The gap determines sleep depth
The two-process model explains not only when you fall asleep – it also explains how deeply: Dijk & Czeisler showed in a landmark 1995 study using a "forced desynchrony" protocol that slow-wave activity (SWA) – the most reliable marker of deep sleep – depends directly on the gap between Process S and Process C.
In the first half of the night this gap is largest: sleep pressure (Process S) is maximal after a long day while circadian wake promotion (Process C) reaches its minimum. The result is a phase of especially deep sleep with high slow-wave activity – precisely the phase in which the most important regenerative processes occur: growth hormones are released, the immune system is strengthened, and the brain performs a kind of "cleansing" via the glymphatic system.
As the night progresses this relationship changes: sleep pressure dissipates with each deep-sleep phase while the internal clock increasingly sends waking signals towards morning. The gap between S and C shrinks – sleep becomes lighter and REM-dominated. In the morning, when the curves meet again, you wake up.
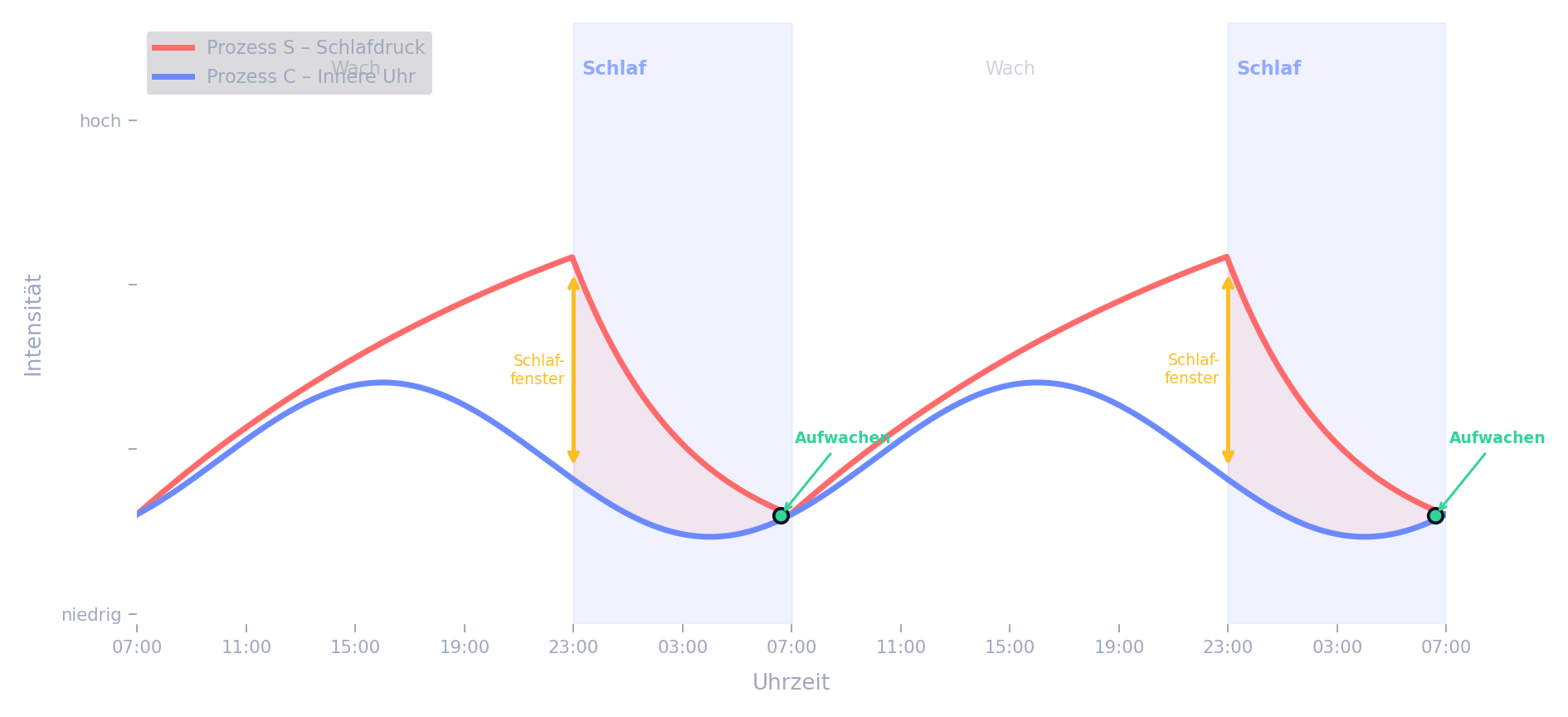
The two-process model by Borbély (1982). Red: Process S (sleep pressure) rises during wakefulness and falls during sleep. Blue: Process C (circadian wake promotion) oscillates independently. The gap between curves during sleep determines sleep depth – the larger the gap, the deeper the sleep (Dijk & Czeisler 1995). Where the curves converge, sleep lightens and ultimately ends with waking.
Core body temperature over 24 hours
The following chart shows the typical course of core body temperature over a day-night cycle. The temperature curve correlates closely with the circadian rhythm (Process C) – it drops in the evening and reaches its minimum in the early morning hours, precisely when deep sleep is most intense.
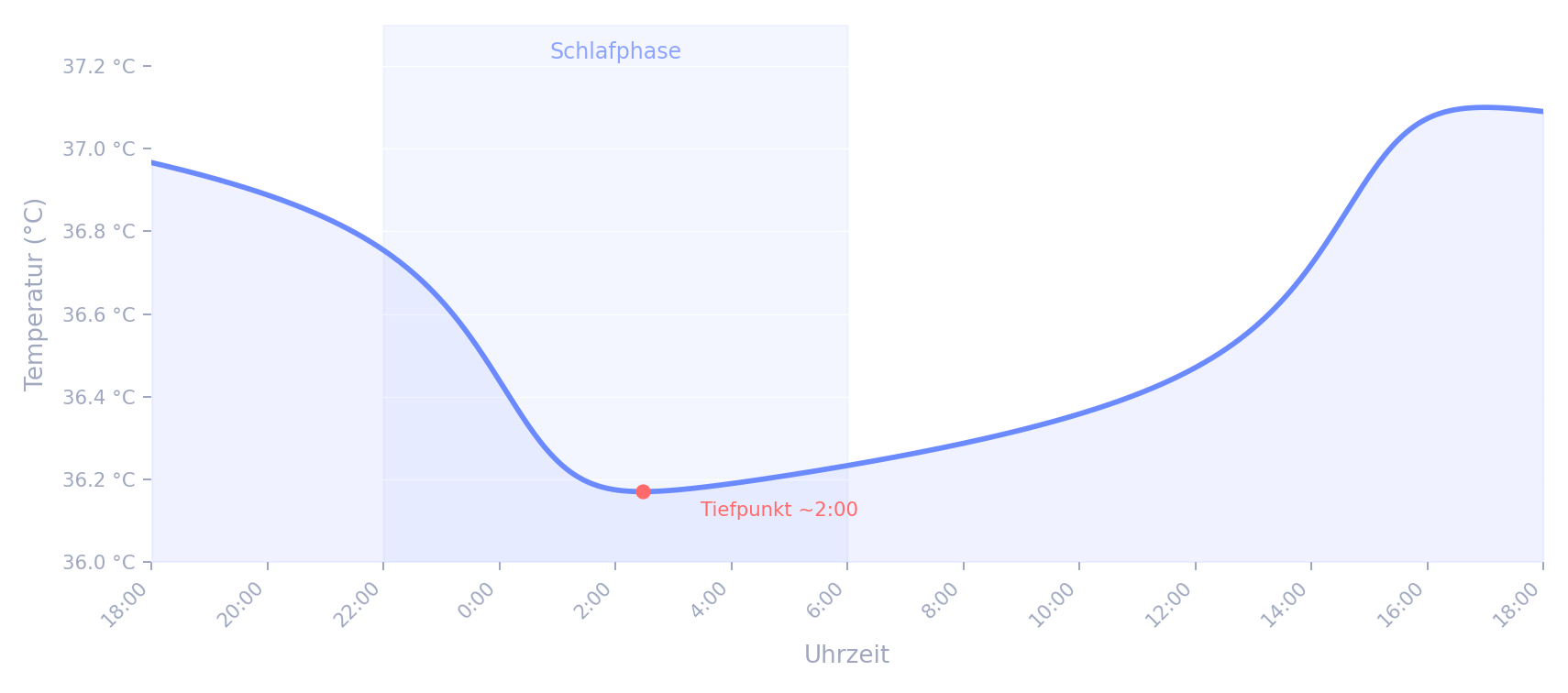
Schematic course of core body temperature over 24 hours. Modelled after the Van der Pol oscillator (Kronauer 1982; Jewett & Kronauer 1999), based on Borbély (1982) and Gilbert et al. (2004).
The evening temperature drop is not random – it is actively controlled by the body. From around 8 pm the blood vessels in the hands and feet begin to dilate (vasodilation). Warm blood from the body core flows to the extremities, where heat is released through the skin to the surroundings. Hands and feet become warm, the core cools.
The sleep-stabilising spiral
The drop in core temperature activates heat-sensitive neurons in the preoptic area of the hypothalamus (POAH). These neurons are a central part of the sleep system: when they register that the body core is cooling, they initiate sleep.
A self-reinforcing spiral emerges:
- The body core cools → heat-sensitive neurons in the POAH are activated
- The neurons initiate sleep → metabolism is further reduced
- Core body temperature drops further → neurons remain active
- Deeper sleep stages are reached and stabilised
Gilbert et al. (2004) describe this coupling as the thermoregulatory sleep signal: peripheral heat dissipation is not merely a side effect but an active signal to the brain to initiate and maintain sleep. If this heat dissipation is disrupted – for example by a too-warm or insulating duvet – sleep pressure may be high but the body cannot enter the deep sleep it needs.
What happens when the spiral is disrupted
Too warm under the duvet: When the ambient temperature is too high, the body core cannot release heat adequately. The sleep-promoting neurons in the POAH are not sufficiently activated. The consequence: difficulty falling asleep, less deep sleep, more frequent waking. The large S–C gap – the foundation for deep sleep – goes unused because the temperature link is missing.
Too cold in the bedroom: The body responds to cold with vasoconstriction – it narrows the blood vessels in the extremities to limit heat loss. But this blocks exactly the mechanism that should lower core temperature. The core stays warm, the sleep signal stays absent. You lie awake even though you are tired.
The ideal sleeping environment is neither too warm nor too cold – it allows the body core to lower its temperature in a controlled way without the extremities cooling too much.
Between freezing and sweating – why our body works differently at night
Podcast interview with sleep researcher Dr. Christine Blume (University of Basel) on Deutschlandfunk Nova. (German)
Related articleAm I affected?
The hidden symptoms of the wrong sleep temperature.
Read moreThe perfect sleep temperature
What research says about the microclimate under your duvet.
Scientific sources for this article
Borbély (1982) – A Two Process Model of Sleep Regulation
Foundational model of sleep regulation: Process S (homeostatic sleep pressure) and Process C (circadian rhythm) work together to control the sleep-wake cycle.
Dijk & Czeisler (1995) – Contribution of the Circadian Pacemaker and the Sleep Homeostat to Sleep Propensity, Sleep Structure, EEG Slow Waves, and Sleep Spindle Activity in Humans
Harvard Medical School. Forced-desynchrony study with 8 subjects: slow-wave activity (deep sleep) is primarily determined by homeostatic sleep pressure, while REM sleep is governed by the circadian rhythm. The S–C gap determines sleep depth – in the first half of the night this gap is maximal, explaining the high concentration of deep sleep.
Gilbert et al. (2004) – Thermoregulation as a Sleep Signalling System
University of South Australia. Peripheral heat dissipation via hands and feet is a central signal for sleep onset. Thermoregulatory centres in the hypothalamus interact directly with sleep-regulating neurons.
Van Someren (2006) – Mechanisms and Functions of Coupling between Sleep and Temperature Rhythms
Sleep preferentially occurs during the circadian phase of reduced heat production and increased heat dissipation – the latter through a strong increase in skin blood flow.
Togo et al. (2007) – Influence on Human Sleep Patterns of Lowering the Minimum Core Body Temperature
Deliberately lowering ambient temperature increased deep sleep duration from 89 to 121 minutes (+36 %). Core body temperature fell by an additional 0.2 °C.
Komagata et al. (2020) – Dynamic REM Sleep Modulation by Ambient Temperature
Thermoregulation is strongly impaired during REM sleep. The MCH system modulates REM sleep expression in dependence on ambient temperature.
Tsuzuki et al. (2018) – The Effects of Low Air Temperatures on Thermoregulation and Sleep
Study at 3 °C, 10 °C and 17 °C room temperature with young men. Sleep quality depended on the microclimate under the duvet and was largely independent of room temperature.